Scar Revision Surgery
Scar revision surgery encompasses a range of precise techniques including Z-plasty, W-plasty and simple excision with meticulous re-closure. These procedures aim to improve the appearance, orientation and suppleness of unsightly or functionally limiting scars so that they blend more naturally with the surrounding skin.
Overview
Scar revision surgery aims to improve the appearance and function of scars that are wide, depressed, raised, discoloured, irregular, tethered or poorly oriented in relation to the natural lines of the skin. While no scar can be completely erased, the goal of revision is to replace an unfavourable scar with one that is narrower, smoother, better positioned and less conspicuous.
Mr Singh will assess the maturity, direction and quality of the existing scar together with the surrounding skin and underlying tissue. Most scars benefit from being allowed to mature for a year or more before revision is considered, as scars often improve significantly during this period. When revision is appropriate, the technique is carefully chosen to address the specific problem whether that be width, irregularity, tension, contracture or a scar that runs against the skin's natural lines.
Benefits
- Improved appearance: A narrower, flatter, better oriented scar that is less noticeable than the original.
- Reorientation: Realignment of scars into the natural creases and tension lines of the skin, where they are much less visible.
- Relief of contracture: Release of tight scars that pull on adjacent structures or restrict movement across joints.
- Improved function: Greater flexibility and range of motion, particularly where scars cross joints or the face.
- Symptomatic improvement: Reduction in discomfort, itching or tenderness associated with some scars.
- Psychological benefit: Greater self-confidence and comfort in social and professional settings.
Surgical Techniques
The technique chosen depends on the size, shape, orientation and cause of the scar, as well as the quality of the surrounding skin. Mr Singh will explain the most appropriate option during your consultation and tailor the plan to your individual anatomy and goals.
- Simple Excision and Re-Closure: The existing scar is carefully excised and the wound closed in layers with fine sutures, allowing a tension-free repair that usually produces a finer scar than the original.
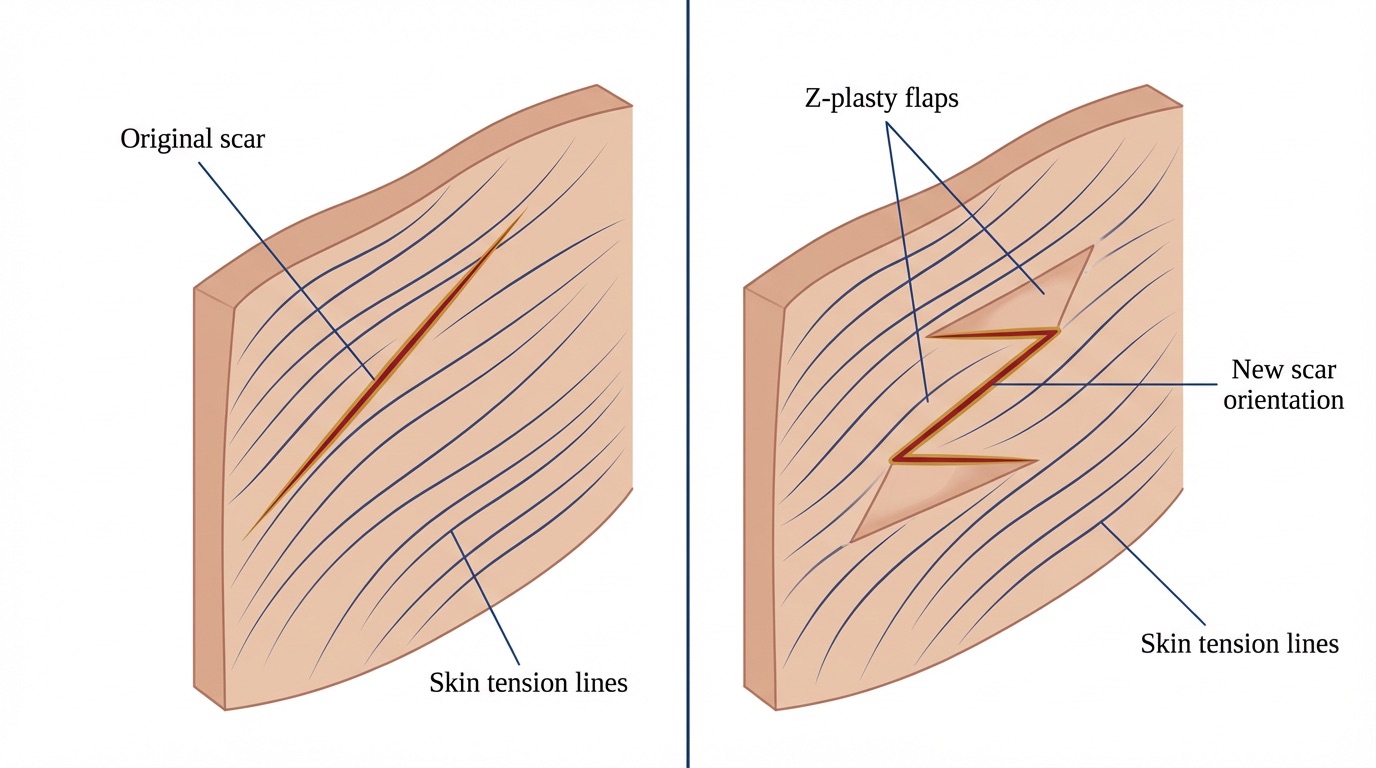
- Z-Plasty: A geometric technique using interposing triangular flaps to change the direction of a scar and lengthen it, particularly useful for tight, contracted scars or scars that cross natural skin creases at an unfavourable angle.
- W-Plasty: A series of small, interlocking triangles are designed along the length of a straight scar, breaking it up into shorter segments that are less conspicuous to the eye.
- Geometric Broken Line Closure: An advanced variation of W-plasty using irregular small shapes to further disguise longer scars on visible areas such as the face.
- Local Flap Rearrangement: For larger or tethered scars, small local flaps of surrounding skin are used to relieve tension and produce a supple, well-contoured result.
- Layered Closure: Irrespective of technique, the wound is closed in multiple layers using dissolvable deep sutures to support the skin edges and fine superficial sutures to give a precise final result.
Risks & Considerations
General Risks
- Infection: Risk of wound infection which can delay healing and may require antibiotics.
- Bleeding and bruising: Minor bleeding or haematoma formation can occur at the surgical site.
- Scarring: Revision surgery always produces a new scar; the goal is to produce a better scar than the original, not to eliminate scarring entirely.
- Anaesthetic risks: Local, regional or general anaesthetic carries its own small set of risks depending on the technique used.
Specific Risks to Scar Revision
- Unpredictable healing: The quality of the new scar depends partly on how an individual's skin heals and cannot be guaranteed in advance.
- Recurrence of widening or thickening: Particularly in high-tension areas such as the chest, shoulders and back.
- Pigmentation changes: Temporary or permanent lightening or darkening of the new scar, more common in darker skin types.
- Numbness: Temporary or permanent loss of sensation in the area of the scar due to disruption of small nerve fibres.
- Wound dehiscence: Separation of the wound edges, particularly if there is tension or excessive early activity.
- Dissatisfaction with the result: Occasionally patients feel the new scar is not significantly better and further revision or non-surgical treatment may be considered.
Recovery
Wound Care
- Dressings: A light dressing or skin tape is applied after surgery and is usually robust enough to tolerate gentle showering. Dressings are typically removed at the first post-operative visit.
- Cleaning: Gently clean the wound with mild soap and water and pat dry. Daily showering is encouraged to reduce the risk of infection.
- Activity: Most daily activities can be resumed within a day or two; strenuous exercise and heavy lifting should be avoided for several weeks to protect the repair.
- Suture Removal: Where non-dissolving sutures are used, these are typically removed between 7 and 14 days depending on the location.
Scar Advice
- Silicone Therapy: Silicone sheets or gel should be started once the wound is fully healed and continued for at least three to six months to optimise the final appearance.
- Sun Protection: New scars must be protected from sun exposure with high-factor sunscreen or clothing for the first 6–8 weeks to prevent pigmentation changes.
- Scar Massage: Once the wound is healed, regular gentle massage with a bland moisturiser helps soften the scar and improve its final texture.
- Taping: Micropore taping may be recommended for several months to support the scar and reduce widening.
Follow-Up
- Initial Post-Op Visit: Typically scheduled around a week after surgery to check wound healing and, where required, remove non-dissolving sutures.
- Subsequent Visits: Usually seen again at around 6 weeks and 3 to 4 months to assess early maturation and provide scar-care advice.
- Long-Term Review: A final review at around 12 months allows the mature result to be assessed, as scars continue to improve for up to a year or longer.
- Long-Term Care: Mr Singh remains available for any concerns or further follow-up as required.
Procedure Summary
Ready to Discuss Scar Revision Surgery?
If you are troubled by an unsightly or uncomfortable scar, please feel free to contact us to answer any questions you may have or to schedule a consultation and learn how scar revision with Mr Singh may benefit you.
Book a Consultation